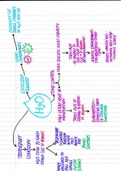
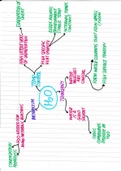
Lecture 1- Chronic diseases
chronic diseases: noncontagious long-term conditions which can often be controlled but not
cured by medications or prevented by vaccinations.
Risk factors: age - elderly → 60% 50+ have cd’s, cardiovascular disease, diabetes
- (behavioral) risk health behaviors : smoking, sedentary, unhealthy diet
Stable (e.g., hypertension) versus progressive (e.g., Alzheimer’s disease)
• Episodic (e.g., relapsing-remitting MS)
• Remission (e.g., RA)
Health psychologist:
• Address barriers for healthy behavior(s); i.e., adherence to medication
• Adjustment, coping
• Psychosocial problems
• Examine psychosocial factors
The biopsychosocial model is a comprehensive approach to understanding health
and illness, integrating biological, psychological, and social factors.
1. biological (genetics, physiology)
2. psychological (behavior, cognition, emotions)
3. social (ses, culture, support)
→ holistic treatment
how everything contributes to condition and progression
→ best for cd’s and conditions with no clear biological cause (fibromyalgia)
Example: Managing Chronic Pain
•A biopsychosocial approach would include:
- Biological Interventions: Medications or physical therapy.
- Psychological Support: Cognitive-behavioral therapy to address negative thoughts and
improve coping mechanisms.
- Social Considerations: Enhancing social support and addressing environmental stressors.
Dominant view physicians (& clients): biomedical models Biomedical model: The physician is
the expert, treating the illness and symptoms, while the client is more passive. Dominant
view psychologists: psychosocial models Psychosocial model: The therapist acts as a
coach, and the client actively works on coping strategies and lifestyle changes; both must
be engaged.
IBS: gastrointestinal disorder affecting the large intestine
Contributing factors:
Medical: past infections can trigger, abnormal muscle contractions of the large intestine lead
to diarrhea or constipation, family history (IBD)
Psychological: stress can trigger/worsen, perception of pain, coping mechanisms
Social: lack of support, stigma, healthcare access
,Impact: anxiety, depression, social withdrawal, - QoL, body image issues
Medical treatment: probiotics, laxatives or antidiarrheals
Psychological treatment: CBT, psychotherapy, stress management
Social: increasing support/ addressing environmental stressors
medical treatment for IBD: anti-inflammatory drugs, surgery, immune system suppressors
• Differences: - Biological Basis IBD: Immune-mediated inflammation and tissue damage.
IBS: Functional disorder with no visible inflammation. - Treatment Focus IBD: Controlling
inflammation and immune responses. IBS: Managing symptoms and psychological triggers.
————
1. Primary prevention: Aims to prevent disease onset through interventions like
lifestyle changes and education.
2. Secondary prevention: Focuses on early detection and treatment to halt disease
progression, such as screenings and adherence to treatment regimens.
3. Tertiary prevention: Aims to reduce complications or recurrence of established
diseases, like chemotherapy or managing diabetes-related complications.
most chronic diseases could be prevented or delayed by addressing modifiable risk factors
Four Pillars of Primary Prevention (4Ps)—tobacco cessation, weight loss, healthy diet,
and regular exercise—as key strategies to prevent chronic diseases. These interventions
form the foundation of primary prevention and have direct and indirect benefits, such as
reducing the risk of type 2 diabetes, cardiovascular disease, and other chronic illnesses.
Adherence to all four behaviors is low, with less than 3% of Americans following them fully.
Key Highlights of Each Pillar: no details needed, read through
1. Tobacco Cessation
○ Smoking causes numerous cancers, heart disease, stroke, and chronic
obstructive pulmonary disease.
○ It is responsible for 90% of lung cancer deaths.
○ Quitting: mmediate and long-term improvements
2. Weight Loss
○ Obesity leads to type 2 diabetes, heart disease, stroke, certain cancers, and
other conditions.
○ Over two-thirds of U.S. adults are overweight or obese, with significant risks
even in children and adolescents.
3. Regular Exercise
○ Recommended: 30–45 minutes of moderate exercise, 3–5 times per week.
○ Exercise reduces the risk of CVD, diabetes, and certain cancers while
improving mood, cholesterol levels, and blood pressure.
○ Yet, 40% of U.S. adults do not engage in regular physical activity, doubling
their risk of coronary heart disease (CHD).
4. Healthy Diet
, ○ Poor dietary choices contribute to obesity, CVD, hypertension, diabetes, and
some cancers.
○ Most Americans consume excessive saturated and trans fats while lacking
sufficient fruits, vegetables, fiber, and low-fat dairy.
○ Adhering to dietary guidelines, including fruits, vegetables, and whole grains,
can lower disease risks and aid weight loss.
Lecture 2- Rheumatic diseases
Chronic pain and rheumatic diseases (chapter 15)
pain: individualized experience, doesn’t always correspond to actual damage
Classifying by…
- Underlying cause:
- nociceptive pain: signals than an injury has occurred, burns/ bruises
- neuropathic: due to damage of the nerves, diabetes/cancer from chemo- radiotherapy
- mixed pain: nociceptive and neuropathic, herniated disk
- nociplastic: altered nociception but without the biological evidence, IBS, fibromyalgia
- idiopathic : no evidence of pathology/injury
- Duration
- Acute: less than 3-6 months
- Chronic: more than 3-6 months (90% no longer associated with injury)
- Frequency
- Brief (bump knee)
- Intermittent (with or without pattern, migraines)
- Constant (chronic back pain)
Unidimensional models
- Biomedical: pain should be proportional to pathology, only sometimes true → medical
treatment
chronic diseases: noncontagious long-term conditions which can often be controlled but not
cured by medications or prevented by vaccinations.
Risk factors: age - elderly → 60% 50+ have cd’s, cardiovascular disease, diabetes
- (behavioral) risk health behaviors : smoking, sedentary, unhealthy diet
Stable (e.g., hypertension) versus progressive (e.g., Alzheimer’s disease)
• Episodic (e.g., relapsing-remitting MS)
• Remission (e.g., RA)
Health psychologist:
• Address barriers for healthy behavior(s); i.e., adherence to medication
• Adjustment, coping
• Psychosocial problems
• Examine psychosocial factors
The biopsychosocial model is a comprehensive approach to understanding health
and illness, integrating biological, psychological, and social factors.
1. biological (genetics, physiology)
2. psychological (behavior, cognition, emotions)
3. social (ses, culture, support)
→ holistic treatment
how everything contributes to condition and progression
→ best for cd’s and conditions with no clear biological cause (fibromyalgia)
Example: Managing Chronic Pain
•A biopsychosocial approach would include:
- Biological Interventions: Medications or physical therapy.
- Psychological Support: Cognitive-behavioral therapy to address negative thoughts and
improve coping mechanisms.
- Social Considerations: Enhancing social support and addressing environmental stressors.
Dominant view physicians (& clients): biomedical models Biomedical model: The physician is
the expert, treating the illness and symptoms, while the client is more passive. Dominant
view psychologists: psychosocial models Psychosocial model: The therapist acts as a
coach, and the client actively works on coping strategies and lifestyle changes; both must
be engaged.
IBS: gastrointestinal disorder affecting the large intestine
Contributing factors:
Medical: past infections can trigger, abnormal muscle contractions of the large intestine lead
to diarrhea or constipation, family history (IBD)
Psychological: stress can trigger/worsen, perception of pain, coping mechanisms
Social: lack of support, stigma, healthcare access
,Impact: anxiety, depression, social withdrawal, - QoL, body image issues
Medical treatment: probiotics, laxatives or antidiarrheals
Psychological treatment: CBT, psychotherapy, stress management
Social: increasing support/ addressing environmental stressors
medical treatment for IBD: anti-inflammatory drugs, surgery, immune system suppressors
• Differences: - Biological Basis IBD: Immune-mediated inflammation and tissue damage.
IBS: Functional disorder with no visible inflammation. - Treatment Focus IBD: Controlling
inflammation and immune responses. IBS: Managing symptoms and psychological triggers.
————
1. Primary prevention: Aims to prevent disease onset through interventions like
lifestyle changes and education.
2. Secondary prevention: Focuses on early detection and treatment to halt disease
progression, such as screenings and adherence to treatment regimens.
3. Tertiary prevention: Aims to reduce complications or recurrence of established
diseases, like chemotherapy or managing diabetes-related complications.
most chronic diseases could be prevented or delayed by addressing modifiable risk factors
Four Pillars of Primary Prevention (4Ps)—tobacco cessation, weight loss, healthy diet,
and regular exercise—as key strategies to prevent chronic diseases. These interventions
form the foundation of primary prevention and have direct and indirect benefits, such as
reducing the risk of type 2 diabetes, cardiovascular disease, and other chronic illnesses.
Adherence to all four behaviors is low, with less than 3% of Americans following them fully.
Key Highlights of Each Pillar: no details needed, read through
1. Tobacco Cessation
○ Smoking causes numerous cancers, heart disease, stroke, and chronic
obstructive pulmonary disease.
○ It is responsible for 90% of lung cancer deaths.
○ Quitting: mmediate and long-term improvements
2. Weight Loss
○ Obesity leads to type 2 diabetes, heart disease, stroke, certain cancers, and
other conditions.
○ Over two-thirds of U.S. adults are overweight or obese, with significant risks
even in children and adolescents.
3. Regular Exercise
○ Recommended: 30–45 minutes of moderate exercise, 3–5 times per week.
○ Exercise reduces the risk of CVD, diabetes, and certain cancers while
improving mood, cholesterol levels, and blood pressure.
○ Yet, 40% of U.S. adults do not engage in regular physical activity, doubling
their risk of coronary heart disease (CHD).
4. Healthy Diet
, ○ Poor dietary choices contribute to obesity, CVD, hypertension, diabetes, and
some cancers.
○ Most Americans consume excessive saturated and trans fats while lacking
sufficient fruits, vegetables, fiber, and low-fat dairy.
○ Adhering to dietary guidelines, including fruits, vegetables, and whole grains,
can lower disease risks and aid weight loss.
Lecture 2- Rheumatic diseases
Chronic pain and rheumatic diseases (chapter 15)
pain: individualized experience, doesn’t always correspond to actual damage
Classifying by…
- Underlying cause:
- nociceptive pain: signals than an injury has occurred, burns/ bruises
- neuropathic: due to damage of the nerves, diabetes/cancer from chemo- radiotherapy
- mixed pain: nociceptive and neuropathic, herniated disk
- nociplastic: altered nociception but without the biological evidence, IBS, fibromyalgia
- idiopathic : no evidence of pathology/injury
- Duration
- Acute: less than 3-6 months
- Chronic: more than 3-6 months (90% no longer associated with injury)
- Frequency
- Brief (bump knee)
- Intermittent (with or without pattern, migraines)
- Constant (chronic back pain)
Unidimensional models
- Biomedical: pain should be proportional to pathology, only sometimes true → medical
treatment