Anaemia: reduction in red blood cell numbers and/or Hb below normal
Epi: most common blood disorder
Ax – blood loss (trauma, surg, haematemesis), reduced production from bone marrow (nutritional deficiencies i.e vegetarian or vegan + Fe, B12, folate; increased demand e.g pregnancy; EPI deficiency i.e ESRF;
haematological malignancy; infection of progenitors e.g parovirus B19 – aplastic anaemia) , increased breakdown
Hx – asymptomatic, fatigue, loss of energy, exertional SOB, dizziness, palpitations, CP if IHD, pallor of mucous membranes
Examination – pallor, conjunctivae first; flow murmur, tachycardia
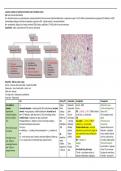
Blood Film – RBC size, colour, shape
Normal – biconcave with central pallor + smaller than WBCs
Spherocytes – loss of central pallor + round + red
Sickle cells – bananas
Tear drops cells – thalassaemia, myelofibrosis
Pencil cells – elliptocytosis
Info History/RF Examination Investigation Management
Iron deficiency Ax – Fatigue Koilonychia Bedside – ECG Address the cause
anaemia Decreased absorption – atrophic gastritis, IBD, coeliac disease; increased Pallor Conjunctival Bloods – 1 Oral Iron Replacement
Hypochromic, demand – during pregnancy, childrens/adolescents; increased loss of Lethargy pallor FBE – ↓Hb/HCr, ↓ MCV, ↑RDW (variation Give w/ Vit C
microcytic anaemia iron – GIT bleeding – right sided colon Ca, PUD, menorrhagia; dietary – Hair loss Hair loss of cell sizes), ↓ reticulocytes AD: Constipation, black
due to low cellular insuffient intake i.e vegetarian or vegan, malnutrition Brittle nails Nail changes UEC stools
iron Prolonged deficiency – depletes iron stores in the body resulting in Pica – thinning, Iron studies – ↓ ferritin, ↑TIBC/↑ 2 Parenteral iron
decreased erythropoiesis and anaemia Palpitations flattening? transferrin, ↓ iron saturation replacement
Most common cause Pathophys – SOB Atrophic Peripheral blood smear – microcytic Superior efficacy to oral
of anaemia Iron deficiency → ↓ binding of iron protoporphyrin → ↓ production of glossitis hypochromic, pencil red cells, target red Indication – absorption
Hb RF – Angular cells, anisocytosis (sizes), poikilocytosis issues, unable to tolerate
Epi – most common cause of anaemia, prevalence highest in children up pregnancy, cheilitis (shapes) oral iron, rapid iron loss,
Hb<130g/L in men
to 5 yrs, young women of reproductive age, pregnant women young EPO – normal or ↑ correction needed quickly
and <120g/L in
children, Tachy Imaging – 3 Red cell transfusion
nonpregnant women
vegetarians Postural Other – Low Hb and Sx – dyspnoea
and <110g/L in
, older pts drop Urea breath test, gastroscopy at rest, CP, pre-syncope
pregnant women
*Ferritin – acute phase reactant i.e Not given at same time as
infection, inflammation, malignancy IV ferritin – too much Fe
, Changing diet if they want?
Could give OCP if primary
cause is menorrhagia
Megaloblastic Ax – vitB12 deficiency – increased use e.g pregnancy; decreased intake – Pallor, SOB, fatigue, Bedside – Urea breath test (exclude iron Treat underlying Ax
Anaemia alcoholism, chronic pancreatitis, vegetarian; impaired absorption – glossitis deficiency anaemia) B12 def – life-long B12
Impairment of DNA intrinsic factor deficiency); malabsorption (coeliac disease); ileal resection Jaundice Bloods – supplementation
synthesis affecting or inflammation (Crohn’s), toxins FBE – ↓Hb, ↑ MCV, +/- ↓WCC, ↓platelets Oral – w/o autoimmune
haematopoesis and Folate deficiency – increased use e.g pregnancy; decreased intake – B12 deficiency – Peripheral Blood Smear – macrocytosis, gastritis
causing a distinct alcoholism, drugs (methotrexate); impaired absorption (coeliac, Crohns, neurological signs as it may hypersegmented neutrophils (6-7 lobes), Parenteral (injection or
morphological change chronic pancreatitis); impaired utilization – folic acid antagonists e.g affect the posterior column ovalocytes, tear drops infusion) – W/
in the RBCs methotrexate or trimethoprim and the corticospinal tract B12 def – ↓B12, ↓ holotranscobalamin autoimmune gastritis
Pathophys – B12 and folate are co-enzymes required for thymidine – changes in reflexes, poor Folate def – ↓ serum folate, ↓ Red cell
Folate – vitB9 synthesis – both are needed for an effective DNA synthesis for RBCs muscle function, memory Folate Blood transfusion if
Deficiency – impairment of cell division → cell grows for too long without problems Intrinsic factor/parietal cell antibodies symptomatic
division → large RBCs = megaloblastosis Neuropsych Sx – Schilling Test – give oral radioactive B12 + Med Hx – antacids, long-
Pregnant woman –
Co-enzymes – even if you supplement one, the other needs to be normal depression, cognitive IM non-radioactive B12 which will flush out term PPI, metformin
impairment in the
for it to work → supplement both slowing, forgetfulness, radiolabelled B12 – THEN 24 hr urine associated w/ reduced B12
closure of anterior
Humans cannot make folate, therefore must come from diet dementia, psychosis collection absorption
and posterior
Pernicious anaemia – from b12 deficiency due to autoimmune gastritis Chronic atrophic gastritis,
neuropore
Antibodies against parietal cells → loss of intrinsic factor → prevents gastric resection
Folate deficiency – no
normal absorption of the IF-B12 complex at the terminal ileum Phenytoin, trimethoprim,
neurological signs
Epi – B12 deficiency is the most common Ax of megaloblastic anaemia sulfasalazine,
methotrexate – interfere
Increased risk of IHD, stroke Trial of B12/Folate supplementation w/ folate absorption
Haemolytic Anaemia Ax – Congenital – Hereditary spherocytosis, G6PD deficiency, pyruvate Pallor CHURBL
Abnormal and kinase deficiency, sickle cell disease, thalassaemia; Acquired – infection, Jaundice Coombs Test (Direct) – Add known anti-
excessive destruction autoimmune, drug-induced, cardiac, haemolytic transfusion reaction, Fatigue human Ab (coombs serum) to pt blood →
of RBCs before their microangiopathic (haemolytic uraemia syndnrome, thrombotic Dyspnoea agglutination – Ab on RBC; detects
normal 120-day life thrombocytopenic purpura), paroxysmal nocturnal haemoglobinuria Dizziness autoimmune haemolytic anaemia
span; encompasses Splenomegaly Haptoglobin binds free Hb → therefore, ↓
several different Fava beans exacerbate G6PD deficiency when a lot of haemolysis (lots of Hb); also
conditions Leg ulcers is an acute phase reactant
Unconjugated hyperbilirubinaemia
Hereditary Spherocytosis – autosomal dominant; disorder of RBC, cells
↑ Reticulocytes
are less deformable, therefore get stuck in blood vessels and are RF – any of the Ax,
Blood film – reticulocytes, RBC fragments,
destroyed by the spleen autoimmune disorders,
Helmet cell (schistocytes), bite cells (small
mechanical prosthetic
piece of RBCs), spherocytes (small dense
heart valves, family origin is
RBC)
Mediterranean, Middle
↑ LDH – cellular breakdown
East, Africa, Asia
+ urinary haemosiderin test – Free Hb →
degraded to alpha-beta dimers → filtered
through the glomerulus → deposited as
haemosiderin → renal tubular cells →
Epi: most common blood disorder
Ax – blood loss (trauma, surg, haematemesis), reduced production from bone marrow (nutritional deficiencies i.e vegetarian or vegan + Fe, B12, folate; increased demand e.g pregnancy; EPI deficiency i.e ESRF;
haematological malignancy; infection of progenitors e.g parovirus B19 – aplastic anaemia) , increased breakdown
Hx – asymptomatic, fatigue, loss of energy, exertional SOB, dizziness, palpitations, CP if IHD, pallor of mucous membranes
Examination – pallor, conjunctivae first; flow murmur, tachycardia
Blood Film – RBC size, colour, shape
Normal – biconcave with central pallor + smaller than WBCs
Spherocytes – loss of central pallor + round + red
Sickle cells – bananas
Tear drops cells – thalassaemia, myelofibrosis
Pencil cells – elliptocytosis
Info History/RF Examination Investigation Management
Iron deficiency Ax – Fatigue Koilonychia Bedside – ECG Address the cause
anaemia Decreased absorption – atrophic gastritis, IBD, coeliac disease; increased Pallor Conjunctival Bloods – 1 Oral Iron Replacement
Hypochromic, demand – during pregnancy, childrens/adolescents; increased loss of Lethargy pallor FBE – ↓Hb/HCr, ↓ MCV, ↑RDW (variation Give w/ Vit C
microcytic anaemia iron – GIT bleeding – right sided colon Ca, PUD, menorrhagia; dietary – Hair loss Hair loss of cell sizes), ↓ reticulocytes AD: Constipation, black
due to low cellular insuffient intake i.e vegetarian or vegan, malnutrition Brittle nails Nail changes UEC stools
iron Prolonged deficiency – depletes iron stores in the body resulting in Pica – thinning, Iron studies – ↓ ferritin, ↑TIBC/↑ 2 Parenteral iron
decreased erythropoiesis and anaemia Palpitations flattening? transferrin, ↓ iron saturation replacement
Most common cause Pathophys – SOB Atrophic Peripheral blood smear – microcytic Superior efficacy to oral
of anaemia Iron deficiency → ↓ binding of iron protoporphyrin → ↓ production of glossitis hypochromic, pencil red cells, target red Indication – absorption
Hb RF – Angular cells, anisocytosis (sizes), poikilocytosis issues, unable to tolerate
Epi – most common cause of anaemia, prevalence highest in children up pregnancy, cheilitis (shapes) oral iron, rapid iron loss,
Hb<130g/L in men
to 5 yrs, young women of reproductive age, pregnant women young EPO – normal or ↑ correction needed quickly
and <120g/L in
children, Tachy Imaging – 3 Red cell transfusion
nonpregnant women
vegetarians Postural Other – Low Hb and Sx – dyspnoea
and <110g/L in
, older pts drop Urea breath test, gastroscopy at rest, CP, pre-syncope
pregnant women
*Ferritin – acute phase reactant i.e Not given at same time as
infection, inflammation, malignancy IV ferritin – too much Fe
, Changing diet if they want?
Could give OCP if primary
cause is menorrhagia
Megaloblastic Ax – vitB12 deficiency – increased use e.g pregnancy; decreased intake – Pallor, SOB, fatigue, Bedside – Urea breath test (exclude iron Treat underlying Ax
Anaemia alcoholism, chronic pancreatitis, vegetarian; impaired absorption – glossitis deficiency anaemia) B12 def – life-long B12
Impairment of DNA intrinsic factor deficiency); malabsorption (coeliac disease); ileal resection Jaundice Bloods – supplementation
synthesis affecting or inflammation (Crohn’s), toxins FBE – ↓Hb, ↑ MCV, +/- ↓WCC, ↓platelets Oral – w/o autoimmune
haematopoesis and Folate deficiency – increased use e.g pregnancy; decreased intake – B12 deficiency – Peripheral Blood Smear – macrocytosis, gastritis
causing a distinct alcoholism, drugs (methotrexate); impaired absorption (coeliac, Crohns, neurological signs as it may hypersegmented neutrophils (6-7 lobes), Parenteral (injection or
morphological change chronic pancreatitis); impaired utilization – folic acid antagonists e.g affect the posterior column ovalocytes, tear drops infusion) – W/
in the RBCs methotrexate or trimethoprim and the corticospinal tract B12 def – ↓B12, ↓ holotranscobalamin autoimmune gastritis
Pathophys – B12 and folate are co-enzymes required for thymidine – changes in reflexes, poor Folate def – ↓ serum folate, ↓ Red cell
Folate – vitB9 synthesis – both are needed for an effective DNA synthesis for RBCs muscle function, memory Folate Blood transfusion if
Deficiency – impairment of cell division → cell grows for too long without problems Intrinsic factor/parietal cell antibodies symptomatic
division → large RBCs = megaloblastosis Neuropsych Sx – Schilling Test – give oral radioactive B12 + Med Hx – antacids, long-
Pregnant woman –
Co-enzymes – even if you supplement one, the other needs to be normal depression, cognitive IM non-radioactive B12 which will flush out term PPI, metformin
impairment in the
for it to work → supplement both slowing, forgetfulness, radiolabelled B12 – THEN 24 hr urine associated w/ reduced B12
closure of anterior
Humans cannot make folate, therefore must come from diet dementia, psychosis collection absorption
and posterior
Pernicious anaemia – from b12 deficiency due to autoimmune gastritis Chronic atrophic gastritis,
neuropore
Antibodies against parietal cells → loss of intrinsic factor → prevents gastric resection
Folate deficiency – no
normal absorption of the IF-B12 complex at the terminal ileum Phenytoin, trimethoprim,
neurological signs
Epi – B12 deficiency is the most common Ax of megaloblastic anaemia sulfasalazine,
methotrexate – interfere
Increased risk of IHD, stroke Trial of B12/Folate supplementation w/ folate absorption
Haemolytic Anaemia Ax – Congenital – Hereditary spherocytosis, G6PD deficiency, pyruvate Pallor CHURBL
Abnormal and kinase deficiency, sickle cell disease, thalassaemia; Acquired – infection, Jaundice Coombs Test (Direct) – Add known anti-
excessive destruction autoimmune, drug-induced, cardiac, haemolytic transfusion reaction, Fatigue human Ab (coombs serum) to pt blood →
of RBCs before their microangiopathic (haemolytic uraemia syndnrome, thrombotic Dyspnoea agglutination – Ab on RBC; detects
normal 120-day life thrombocytopenic purpura), paroxysmal nocturnal haemoglobinuria Dizziness autoimmune haemolytic anaemia
span; encompasses Splenomegaly Haptoglobin binds free Hb → therefore, ↓
several different Fava beans exacerbate G6PD deficiency when a lot of haemolysis (lots of Hb); also
conditions Leg ulcers is an acute phase reactant
Unconjugated hyperbilirubinaemia
Hereditary Spherocytosis – autosomal dominant; disorder of RBC, cells
↑ Reticulocytes
are less deformable, therefore get stuck in blood vessels and are RF – any of the Ax,
Blood film – reticulocytes, RBC fragments,
destroyed by the spleen autoimmune disorders,
Helmet cell (schistocytes), bite cells (small
mechanical prosthetic
piece of RBCs), spherocytes (small dense
heart valves, family origin is
RBC)
Mediterranean, Middle
↑ LDH – cellular breakdown
East, Africa, Asia
+ urinary haemosiderin test – Free Hb →
degraded to alpha-beta dimers → filtered
through the glomerulus → deposited as
haemosiderin → renal tubular cells →