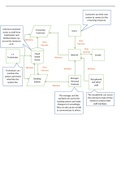
Cardiac monitor = 1 angle of the heart
ECG = views all angles of the heart
1 Small Box = 0.04 sec
1 Big Box = 0.20 sec
5 Small Boxes = 1 Big Box
Repolarization = Resting
Depolarization = Contracting
Intrinsic rates of the conductive system:
o SA Node working = 60 – 100 times/min
o AV Node working = 40 – 60 times/min
o Purkinje Fibers working = 20 – 40 times/min
NORMAL SINUS RHYTHIM
Calculating HR: 60 – 100
o Count # of R’s
o Multiply by 10
If AV node stops working HR: 40 – 60
ST segment always has to be at the isoelectric line, any changes indicates damage to heart
o Up : Acute damage (MI)
o Down : Old damage (ischemia)
Always need to have:
o 1 P wave
o 1 QRS interval
o 1 ST segment
o R-to-R equal
Description Duration
P wave Atriums Depolarization 0.6 – 0.12
PR interval Electricity from SA to AV node 0.12 – 0.20
QRS complex Ventricle Depolarization < 0.12 secs
T wave Ventricle Repolarization 0.16
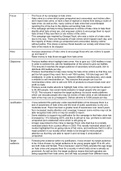
, SINUS BRADYCARDIA
Notes:
Rate < 60
Regular rhythm
Need to have
o 1 P wave
o 1 QRS interval
o 1 T wave
Causes:
Sleeping
Carotid sinus massage
Valsalva maneuver
Hypothermia
Vagal stimulation
Healthy individual (Marathon runner)
Taking certain medication (Beta-Blockers, Calcium Channel Blocker)
Certain diseases:
o MI
o ICP (intracranial pressure)
o Hypothyroidism
Signs/Symptoms: Patient can be asymptomatic or symptomatic
Fatigue Interventions/Treatment:
Weakness If Symptomatic & STABLE (vitals abnormal):
Syncope o Cardiac monitor
Dizziness o Determine underlying cause
Pale o Medications: if CANNOT determine underlying
Cool skin cause
Lethargy
Atropine 0.5 mg IV push
SOB
If Symptomatic & UNSTABLE (vitals abnormal):
Confusion
Hypotension o PACER (for slow HR with pulse)
Chest pain (due to tissue perfusion)
, SINUS TACHYCARDIA
Notes:
Rate > 100
Regular rhythm
Need to have:
o 1 P wave
o 1 QRS interval
o 1 T wave
Causes:
Fever
Exercise
Pain or fear
Anemia
Hypoxia
Dehydration or Fluid volume deficit
Anxiety
Caffeine Interventions/Treatment:
Elicit drugs If Symptomatic:
Hypoxia o Cardiac monitor
Electrolyte imbalances o Determine underlying cause only, no electricity
Taking certain medication (Albuterol, Atropine, Epi, Norepi) o Medications:
Certain diseases: Beta-Blockers (slows HR only)
o Heart failure Be careful with asthma patients
o Pulmonary embolism o Asthma patients need to take selective B-Blockers
o Hyperthyroidism
Beta-Blockers
Signs/Symptoms: Non-Selective: 1st generation Selective: 2nd generation
Anxiety Block both beta 1 (β1) & Block only beta 1 (β1)
Palpitations beta 2 (β2) receptors receptors
SOB/dyspnea o Affect lungs & o Affect only the
Chest pain (due to tissue perfusion) heart heart & CO
Propranolol Metoprolol
Nadolol Acebutolol
Timolol Bisoprolol fumarate
Penbutolol Esmolol
Sotalol Hydrochloride Betaxolol
Pindolol Acebutolol
ECG = views all angles of the heart
1 Small Box = 0.04 sec
1 Big Box = 0.20 sec
5 Small Boxes = 1 Big Box
Repolarization = Resting
Depolarization = Contracting
Intrinsic rates of the conductive system:
o SA Node working = 60 – 100 times/min
o AV Node working = 40 – 60 times/min
o Purkinje Fibers working = 20 – 40 times/min
NORMAL SINUS RHYTHIM
Calculating HR: 60 – 100
o Count # of R’s
o Multiply by 10
If AV node stops working HR: 40 – 60
ST segment always has to be at the isoelectric line, any changes indicates damage to heart
o Up : Acute damage (MI)
o Down : Old damage (ischemia)
Always need to have:
o 1 P wave
o 1 QRS interval
o 1 ST segment
o R-to-R equal
Description Duration
P wave Atriums Depolarization 0.6 – 0.12
PR interval Electricity from SA to AV node 0.12 – 0.20
QRS complex Ventricle Depolarization < 0.12 secs
T wave Ventricle Repolarization 0.16
, SINUS BRADYCARDIA
Notes:
Rate < 60
Regular rhythm
Need to have
o 1 P wave
o 1 QRS interval
o 1 T wave
Causes:
Sleeping
Carotid sinus massage
Valsalva maneuver
Hypothermia
Vagal stimulation
Healthy individual (Marathon runner)
Taking certain medication (Beta-Blockers, Calcium Channel Blocker)
Certain diseases:
o MI
o ICP (intracranial pressure)
o Hypothyroidism
Signs/Symptoms: Patient can be asymptomatic or symptomatic
Fatigue Interventions/Treatment:
Weakness If Symptomatic & STABLE (vitals abnormal):
Syncope o Cardiac monitor
Dizziness o Determine underlying cause
Pale o Medications: if CANNOT determine underlying
Cool skin cause
Lethargy
Atropine 0.5 mg IV push
SOB
If Symptomatic & UNSTABLE (vitals abnormal):
Confusion
Hypotension o PACER (for slow HR with pulse)
Chest pain (due to tissue perfusion)
, SINUS TACHYCARDIA
Notes:
Rate > 100
Regular rhythm
Need to have:
o 1 P wave
o 1 QRS interval
o 1 T wave
Causes:
Fever
Exercise
Pain or fear
Anemia
Hypoxia
Dehydration or Fluid volume deficit
Anxiety
Caffeine Interventions/Treatment:
Elicit drugs If Symptomatic:
Hypoxia o Cardiac monitor
Electrolyte imbalances o Determine underlying cause only, no electricity
Taking certain medication (Albuterol, Atropine, Epi, Norepi) o Medications:
Certain diseases: Beta-Blockers (slows HR only)
o Heart failure Be careful with asthma patients
o Pulmonary embolism o Asthma patients need to take selective B-Blockers
o Hyperthyroidism
Beta-Blockers
Signs/Symptoms: Non-Selective: 1st generation Selective: 2nd generation
Anxiety Block both beta 1 (β1) & Block only beta 1 (β1)
Palpitations beta 2 (β2) receptors receptors
SOB/dyspnea o Affect lungs & o Affect only the
Chest pain (due to tissue perfusion) heart heart & CO
Propranolol Metoprolol
Nadolol Acebutolol
Timolol Bisoprolol fumarate
Penbutolol Esmolol
Sotalol Hydrochloride Betaxolol
Pindolol Acebutolol