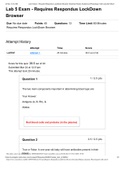
Cataract
The lens is in the anterior segment of the eye, live epithelial cells are compacted into the
nucleus of the lens, these transparent cells denature with age which is what causes the lens
opacity
Risks:
Age
Smoking
Alcohol
Dehydration
Radiation
Diabetes
Steroids (asthsmatics commonly present earlier in life)
Most common is nuclear cataract
Cortical- peripheral lens more loose and can get opacified
PSC- under posterior capsule, common in diabetics and steroid users
Christmas tree- not as common (diabetics and myotonic dystrophies)
Clinical assessment
Visual needs*- if px is non driver may not need to be 6/12
Refraction- astigmatism?
Systemic drugs- alpha agonists affect pupil dilation, tamsulosin- contraindicated in
cataract surgery as can cause floppy iris syndrome (can be accounted for with iris
hooks but surgeon needs to know beforehand so not on referral)
Px needs to lie flat- COPD, spinal abnormalities like ankylosing spondylitis
Deep set eyes- access problems
Blepharitis/lid malposition’s- increased risk of infection
Cornea: Fuchs’- endothelium may need protected
Poor pupil dilation?
Biometry used to determine the IOL power needed from the corneal power and axial length
Phacoemulsification: 2.8mm incision made at limbus, capsule stained blue, ~6mm tear In
the anterior capsule, nucleus emulsified by division into 4, peripheral fibres are younger
fibres, IOL put in and unfolds. Fluid used to AC and lens capsule open until IOL implanted.
Tropicamide and phenylephrine combination usually used (works on the 2 different iris
muscles and gets pupil as big as possible)
Capsularhexis: lens capsule with nucleus inside, we essentially want to deal with the nucleus
and protect the capsule, take old lens away and put new lens inside the lens capsule, access
to nucleus from a tear in lens capsule.
Intraoperative complications:
Posterior capsular tear
Nucleus drop
Zonular dehiscence
, Post op treatment:
Topical streroids (dexamethasome or prednisolone) qds x 4 weeks
Topical antibiotics (chloramphenicol) qds x 4 weeks
If diabetic- topical NSAID
If a patient attended with reduced vision post op- possible CMO
Dilation is safe- every px who has an IOL has a wide open angle because it is thinner than
the normal lens so nothing is pushing the iris forward.
Refractive surgery
1) Laser vision correction
2) IOL
3) Refractive lens exchange
If px is seeking an alternative to contact lenses or glasses can discuss refractive procedures
Cataract surgery “during surgery the surgeon will remove the cloudy lens from the eye and
replace it with an artificial lens which is called an IOL. The surgery usually takes less than an
hour, you will usually be awake and under local anaesthetic”
Refractive consultation
H&S- Motivation for procedure
Refraction
Few years rx history needed
All px’s dilated
Full ophthalmic exam
If px wears CLs make aware they need to be left out 7 days before
Diagnostic scans to give info if px is ok for surgery
Pentacam- corneal curvature
OCT
IOL master- which lens is suited
Factors to take into consideration
Corneal tissue thickness
Post surgery referred to as residual stromal bed- how much tissue left after rx has been
removed
Lasik >540
LASEK > 380
Need to know so we ensure we have enough tissue thickness for surgery
LASIK
The lens is in the anterior segment of the eye, live epithelial cells are compacted into the
nucleus of the lens, these transparent cells denature with age which is what causes the lens
opacity
Risks:
Age
Smoking
Alcohol
Dehydration
Radiation
Diabetes
Steroids (asthsmatics commonly present earlier in life)
Most common is nuclear cataract
Cortical- peripheral lens more loose and can get opacified
PSC- under posterior capsule, common in diabetics and steroid users
Christmas tree- not as common (diabetics and myotonic dystrophies)
Clinical assessment
Visual needs*- if px is non driver may not need to be 6/12
Refraction- astigmatism?
Systemic drugs- alpha agonists affect pupil dilation, tamsulosin- contraindicated in
cataract surgery as can cause floppy iris syndrome (can be accounted for with iris
hooks but surgeon needs to know beforehand so not on referral)
Px needs to lie flat- COPD, spinal abnormalities like ankylosing spondylitis
Deep set eyes- access problems
Blepharitis/lid malposition’s- increased risk of infection
Cornea: Fuchs’- endothelium may need protected
Poor pupil dilation?
Biometry used to determine the IOL power needed from the corneal power and axial length
Phacoemulsification: 2.8mm incision made at limbus, capsule stained blue, ~6mm tear In
the anterior capsule, nucleus emulsified by division into 4, peripheral fibres are younger
fibres, IOL put in and unfolds. Fluid used to AC and lens capsule open until IOL implanted.
Tropicamide and phenylephrine combination usually used (works on the 2 different iris
muscles and gets pupil as big as possible)
Capsularhexis: lens capsule with nucleus inside, we essentially want to deal with the nucleus
and protect the capsule, take old lens away and put new lens inside the lens capsule, access
to nucleus from a tear in lens capsule.
Intraoperative complications:
Posterior capsular tear
Nucleus drop
Zonular dehiscence
, Post op treatment:
Topical streroids (dexamethasome or prednisolone) qds x 4 weeks
Topical antibiotics (chloramphenicol) qds x 4 weeks
If diabetic- topical NSAID
If a patient attended with reduced vision post op- possible CMO
Dilation is safe- every px who has an IOL has a wide open angle because it is thinner than
the normal lens so nothing is pushing the iris forward.
Refractive surgery
1) Laser vision correction
2) IOL
3) Refractive lens exchange
If px is seeking an alternative to contact lenses or glasses can discuss refractive procedures
Cataract surgery “during surgery the surgeon will remove the cloudy lens from the eye and
replace it with an artificial lens which is called an IOL. The surgery usually takes less than an
hour, you will usually be awake and under local anaesthetic”
Refractive consultation
H&S- Motivation for procedure
Refraction
Few years rx history needed
All px’s dilated
Full ophthalmic exam
If px wears CLs make aware they need to be left out 7 days before
Diagnostic scans to give info if px is ok for surgery
Pentacam- corneal curvature
OCT
IOL master- which lens is suited
Factors to take into consideration
Corneal tissue thickness
Post surgery referred to as residual stromal bed- how much tissue left after rx has been
removed
Lasik >540
LASEK > 380
Need to know so we ensure we have enough tissue thickness for surgery
LASIK